 |
August 2014
|
August 2014 // Volume 52 // Number 4 // Research In Brief // v52-4rb1
A Participatory Approach to FCS Food, Nutrition, and Wellness Program Planning
Abstract
To help fill programming gaps in a more organized and collaborative manner, a participatory approach to program planning was tested in Virginia. Programming gaps related to food, nutrition, and wellness programs were filled through a participatory process that involved: an online needs assessment survey; a systematic review of evidence- and practice-based programs; a webinar providing an overview of possible programs for adoption; a program ranking survey; development of an evaluation template; a training; and feedback survey. Our results indicate that a systematic, team-based approach to program planning may be beneficial in guiding trainings and dissemination of programs within Extension.
Introduction
Since the concept was introduced in the 1970s, there has been increasing interest in "participatory" approaches for soliciting behavior change among individuals and communities (Duraiappah, Roddy, & Parry, 2005; "Participatory Approaches," 2007), though they have not been formally used or tested within the Extension framework. In contrast to top-down approaches, participatory approaches aim to maximize involvement of all participants in all steps and processes of a designated project, based on the expectation that people are more likely to actively participate and sustain such projects that incorporate their own perspectives and priorities (Duraiappah et al., 2005; "Participatory Approaches," 2007).
According to self-efficacy theory, an individual's beliefs about his or her abilities to successfully accomplish certain tasks or demonstrate certain behaviors determines whether or not he/she will attempt a certain task or behavior, the amount of effort that will be exerted, and how long the behavior will continue despite obstacles (Bandura, 1978). Learners and educators alike will be more likely to attempt, persevere, and be successful at tasks at which they have a sense of efficacy (Bandura, 1978). Self-efficacy has a strong, positive relationship with work performance (Stajkovic & Luthans, 1998) and is a powerful force in learning and motivation (Bandura, 1978). Motivation is another key factor for adult engagement in learning and sharing knowledge and is enhanced when adults are involved in the planning and evaluation phases of learning (Knowles, 1984). Participatory approaches within Extension could ideally help build self-efficacy and motivation among Extension Educators.
Several studies show participatory approaches contribute to improved project management and have the potential to strengthen rapport and build partnerships between resource holders and beneficiaries ("Participatory Approaches," 2007). The level and type of participation varies among research studies. However, in order for a project to be participatory, it's agreed that stakeholders share control over the decisions and resources that affect them. Translating the participatory process to Extension means that all participants, in this case Family and Consumer Sciences (FCS) agents, are included in program selection and evaluation processes. The hypothesis was that a participatory approach to program planning would help organize, select, and evaluate programs in a collaborative manner that might renew and improve agent interest and engagement in program delivery and promote partnerships among agents and specialists.
Purpose and Objectives
The overall goal of the project reported here was to test a more coordinated, team-based approach to program planning, development, and evaluation. Secondary goals were to improve agent interest and engagement in program delivery and nurture positive specialist-agent partnerships. The objectives of the effort were to: 1) assess program gaps related to food, nutrition, and wellness; 2) identify science- and practice-based programs that would fill these gaps; 3) communicate findings with agents for input; 4) provide trainings, resources, and evaluation tools aligned with those programs; and 5) evaluate feedback from agents.
Methods
Assessment of Program Gaps
In order to assess gap areas and prioritize program needs, an expert validated needs assessment survey was created by a newly formed VCE Food, Nutrition, and Wellness Leadership Team. The SSL online survey was distributed to all 34 Virginia FCS agents through the Extension Listserv. Topic areas included in the needs assessment survey were as follows: kindergarten and 1st grade children; middle school children; teens/adolescents; sports nutrition, and injury prevention for athletes; families (parents with children); hypertension prevention; osteoporosis prevention; Type 2 diabetes prevention; weight loss/ weight maintenance for adults; aging audiences/ seniors. The survey asked agents to rank programming gaps on a scale of 1-5 (1 being not at all important and 5 being an extremely important topic that needs to be addressed in their locality).
Identification of Science- and Practice- based Programs
In order to identify successful programs for the top three gap areas, a comprehensive review of the scientific literature and existing Extension programs was conducted using a combination of PubMed, Google Scholar, and Extension listserv. The characteristics of all programs were summarized and organized into an excel document, including program goals, number of lessons and topics, outcomes and effectiveness, and if tested with Extension. The manuals needed to deliver the programs were retrieved through correspondence with the authors of the research articles and agents who solicited programs through the Listserv.
Communicating Programs with Agents
Potential programs were shared with FCS agents through a webinar and email communication, which included the excel sheet summary of program characteristics. Agents then ranked those programs in terms of how well the programs fit their needs on a scale of 1-5 (1 being absolutely does not fit needs and 5 being completely fits needs), the feasibility in delivering the program on a scale of 1-5 (1 being not at all feasible and 5 being definitely feasible), and finally their preferred choice in programs for each gap area using a SSL online survey.
Program Training, Evaluation, and Feedback
Hands-on trainings were provided by agents and specialists at a statewide training for FCS agents. Simple evaluation indicators and evaluation instrument developed by the VCE Food, Nutrition and Wellness Leadership Team were also provided for agents to assess the outcomes of their participants after program delivery. A final online survey was administered to get feedback on each step as well as the overall participatory process. The questionnaire was developed specifically for the purpose of the study, with content validity achieved by obtaining feedback on the instrument by the Leadership Team. Reliability was not tested, however.
The steps that were evaluated included the initial needs assessment survey (for ranking top nutrition programming gaps); webinar (as an introduction to programs); excel document (as an outline of programs); ranking survey (as a means of voting on programs); training process; and program curricula. The questionnaire asked agents to rank their attitudes towards each step of the participatory approach on a scale of 1-5 (1 being did not like at all and 5 being liked very much) and then to rank the quality of each step of the participatory approach on a scale of 1-5 (1 being poor and 5 being excellent). The final question in the feedback survey asked agents to check off any and all attributes they liked about this approach from a selection of choices. Space for comments and suggestions for improvement were also provided to ensure the best feedback.
Data Collection and Analysis
The online software tool (SurveyMonkey) was used to collect all data and compute the final results. Microsoft Excel (2010) was used to create tables.
Results
Assessment of Program Gaps
With a response rate of 64.7%, 22 agents completed the initial needs assessment survey. The top three programming gaps were identified as: families with children; aging/seniors; and weight management among adults. On a scale from 1 to 5 in levels of importance (1 being least important and 5 being most important), 17 respondents (77.3%) ranked families with children at a level 5. Nineteen respondents ranked aging audiences at a level 4 (57.1%) and level 5 (33.3%). Sixteen respondents ranked weight management at a level 5 (42.9%) and level 4 (33.3%). Type 2 diabetes prevention also scored high, with the majority of respondents at a level 5 (57.1%) or level 4 (28.6%). Because Virginia Cooperative Extension had received NIH funding support for the Dining with Diabetes program, however, the other steps of the process were not conducted for this topic area. The lowest rankings for perceived importance were osteoporosis prevention (71.4% of rankings at levels 1-3) and sports nutrition/injury prevention (85% of rankings at levels 1-3).
Identification of Science- and Practice-Based Programs
The Leadership Team analyzed and discarded some of the initial programs found through the literature review for various reasons, including expense, resources, and/or time commitment, resulting in eight programs for final review by agents.
Program choices for "families with children" included:
- Parenting, Eating, and Activity for Child Health (PEACH) (Magarey et al., 2011)
- Smart Choices for Healthy Families (Pinard et al., 2012)
- Healthy Children, Healthy Families: Parents Making a Difference! (CHANCE) (Lent, Hill, Dollahite, Wolfe, & Dickin, 2012)
Program choices for "aging audiences" included:
- Eat Better & Move More (EBMM) (Wellman, Kamp, Kirk-Sanchez & Johnson, 2007)
- Partners in Wellness (PIW) (Mitchell, Ash & McClelland, 2006)
- Elder Nutrition and Food Safety (ENAFS) (Bobroff et al., 2003)
Program choices for "weight management" included:
- Weight Wise (Samuel-Hodge et al., 2009)
- Reshape Yourself ("Reshape Yourself," 2006)
Communicating Programs with Agents
With a response rate of 50%, 11 of the 22 agents who completed the initial needs assessment survey participated in the ranking survey following the webinar and comprehensive excel sheet that provided information on goals, number of lessons, topics, target audience, study design, outcomes, and effectiveness of programs. The chosen programs based on agent votes included: Smart Choices for Healthy Families; Eat Better & Move More; and Reshape Yourself. Rankings for "families with children" by response count were as follows: PEACH: 1/11 (10%); CHANCE: 3/11 (30%); and Smart Choices for Healthy Families: 6/11 (60%). Rankings for "aging audiences" included: EBMM: 5/11 (45.5%); PIW: 3/11 (27.3%); and ENAFS: 3/11 (27.3%). And rankings for "weight management" included: Weight Wise: 4/11 (36.4%) and Reshape Yourself: 7/11 (63.6%). An additional program, Eat Healthy, Be Active, was introduced after the webinar and was ultimately chosen in place of Reshape Yourself primarily due to administration costs.
Program Training, Evaluation and Feedback
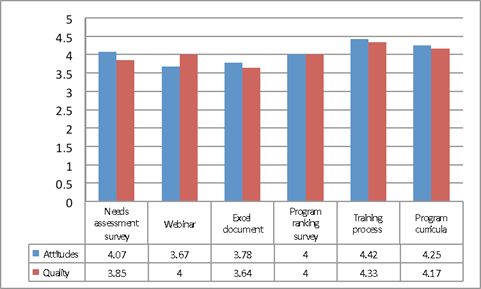
Agents were extremely positive and receptive to the participatory approach at the VCE Food, Nutrition, and Wellness Training in Charlottesville, Virginia. Of the 22 agents who completed the needs assessment survey, 14 (63.6%) completed the feedback survey. The final survey asked agents to rank their attitudes towards each step of the participatory process and then to rank the quality of each component in the participatory process (Figure 1). The agents ranked the training process the highest, followed by the needs assessment survey.
Figure 1.
FCS Agent Feedback on Participatory Processes
With check-all-that-apply, nine (64%) respondents indicated that, "This approach makes it easier to document impacts at statewide levels," and "I liked being a part of the decision-making for programs"; eight (57%) replied that, "This approach will lead to a more coordinated approach to address food, nutrition, and wellness issues"; and seven (50%) answered that, "I appreciated feeling part of a larger effort." Six respondents (43%) reported the approach was more efficient and less work and that they were motivated to deliver these programs, as well as more programs, than when they have no input.
Limitations
Several limitations should be noted. First, many "evidence based" programs identified through the literature review were not necessarily consistent with Extension goals, missions, and capacities, highlighting the challenge in translating tested programs to the Extension system. Second, although we attempted to be as inclusive and participatory as possible, not all agents completed or participated in all components of the project. For example, the response rate was about 68% for the initial needs survey, 50% for the ranking survey, and 63% for the final feedback survey. Because the initial survey was sent to all FCS agents and not all FCS agents teach food, nutrition, and wellness, this may account for the less than 100% participation in the initial survey. Finally, given the small sample size, statistical tests could not be conducted to test hypotheses. Reliability, as well as other forms of validity, were also not conducted.
Conclusions & Implications for Research and Practice
The participatory approach to program planning provides agents with the tools and resources to adopt and deliver new food, nutrition, and wellness programs, consistent with their programmatic needs. Interestingly enough, attitudes towards the webinar and excel document were the lowest (although not low). Because these were the most research-intensive components of the project, perhaps agents felt less comfortable with them. Although the quality of the webinar scored relatively high, the lower score for the excel document may be attributed to it being less "user friendly." Still, the training process obtained the highest scores, suggesting that while specific dimensions may not have been endorsed as much, agents overall approved the participatory process.
This team-based planning required more engagement and commitment from agents than approaches used in the past. Although all agents were informed of the approach, timeline, and process to encourage buy-in and response rate, the communication was predominately through email. More creative approaches to accomplish this are warranted to explicitly describe our goals. Second, administrators were not actively involved in the process. Future initiatives should ensure that administration at the state, district/region, and local levels are aware of the "process" and expectation of all team members to help nudge and encourage participation in the process. Creating a guide for Extension on how to formally establish participatory teams would help Educators with programming and evaluation across program areas.
A participatory approach may be helpful in guiding future trainings and program dissemination within other Extension programming areas in Virginia and across the country. The long-term impacts of participatory engagement on program adoption, delivery, and effectiveness will need to be assessed.
References
Bandura, A. (1978). Self-efficacy: Toward a unifying theory of behavioral change. Advances in Behaviour Research and Therapy, 1(4), 139-161.
Bobroff, L. B., Turner, E., Weddle, D. O., Brake, J. H., Lieberman, L. S., & Allen, T. B. (2003).Interactive learning for congregate nutrition site nutrition education: a pilot study. Journal of Nutrition for the Elderly, 23(1):81-93. doi: 10.1300/J052v23n01_06
Duraiappah, A. K., Roddy, P., & Parry, J. E. (2005). Have participatory approaches increased capabilities? International Institute for Sustainable Development (IISD). Retrieved from: http://www.iisd.org/pdf/2005/economics_participatory_approaches.pdf
Eat Healthy, Be Active Community Workshops. (n.d.). Retrieved from: http://www.health.gov/dietaryguidelines/workshops/?source=govdelivery
Knowles, M. S. (1984). Andragogy in action. Applying modern principles of adult education. San Francisco: Jossey Bass.
Lent, M., Hill, T. F., Dollahite, J. S., Wolfe, W. S., & Dickin, K. L. (2012). Healthy children, healthy families: Parents making a difference! A curriculum integrating key nutrition, physical activity, and parenting practices to help prevent childhood obesity. Journal of Nutrition Education and Behavior, 44(1):90-2.
Magarey, A.M., Perry, R. A., Baur, L.A., Steinback, K.S., Sawyer, M., Hills, A.P.,… Daniels, L.A.(2011) A parent-led family-focused treatment program for overweight children aged 5 to 9 years: the PEACH RCT. Pediatrics, 127(2):214-22.
Mitchell, R. E., Ash, S. L., & McClelland, J. W. (2006). Nutrition education among low-income older adults: A randomized intervention trial in congregate nutrition sites. Health Education & Behavior, 33(3):374-92.
Participatory approaches in health promotion and planning: A literature review. (2007). Retrieved from: http://www.nice.org.uk/aboutnice/whoweare/aboutthehda/hdapublications/participatory_approaches_in_
health_promotion_and_planning__literature_review.jsp
Pinard, C. A., Hart, M. M., Hodgkins, Y., Serrano, E. L., McFerren, M. M., & Estabrooks, P. A. (2012). Smart choices for healthy families: A pilot study for the treatment of childhood obesity in low-income families. Health Education & Behavior. 39(4):433-45. doi: 10.1177/1090198111425686.
Reshape yourself: Promotes healthy lifestyle.(2006). Retrieved from: http://www.uaex.edu/benton/AboutUs/impacts/reshape.htm.
Samuel-Hodge, C. D., Johnston, L. F., Gizlice, Z., Garcia, B. A., Lindsley, S. C., Bramble, K. P.,... Keyserling, T.C . (2009). Randomized trial of a behavioral weight loss intervention for low-income women: the Weight Wise Program. Obesity (Silver Spring), 17(10):1891-9. doi: 10.1038/oby.2009.128.
Stajkovic, A. D., & Luthans, F. (1998). Self-efficacy and work-related performance: A meta-analysis. Psychological bulletin, 124(2), 240.
Wellman, N. S., Kamp B., Kirk-Sanchez, N. J., & Johnson, P. M. (2007). Eat better & move more: a community-based program designed to improve diets and increase physical activity among older Americans. American Journal of Public Health, 97(4):710.




